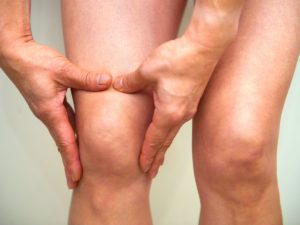
 Osteoarthritis (degenerative joint disease or osteoarthrosis) is the most common form of arthritis, affecting millions of people around the world. Often called wear-and-tear arthritis, osteoarthritis occurs when the protective cartilage on the ends of bones wears down over time. It causes pain, swelling and reduced motion in your joints.
Osteoarthritis (degenerative joint disease or osteoarthrosis) is the most common form of arthritis, affecting millions of people around the world. Often called wear-and-tear arthritis, osteoarthritis occurs when the protective cartilage on the ends of bones wears down over time. It causes pain, swelling and reduced motion in your joints.
Osteoarthritis (OA) can occur in any joint, but usually it affects your hands, knees, hips or spine. Osteoarthritis involves the entire joint, including the nearby muscles, underlying bone, ligaments, joint lining (synovium), and the joint cover (capsule). A variety of causes—hereditary, developmental, metabolic, and mechanical—may initiate processes leading to loss of cartilage.
Osteoarthritis mostly affects cartilage, the hard but slippery tissue that covers the ends of bones where they meet to form a joint. Healthy cartilage allows bones to glide over one another. It also absorbs energy from the shock of physical movement. In osteoarthritis, the surface layer of cartilage breaks and wears away. This allows bones under the cartilage to rub together, causing pain, swelling, and loss of motion of the joint. Over time, the joint may lose its normal shape. Also, small deposits of bone—called osteophytes or bone spurs—may grow on the edges of the joint. Bits of bone or cartilage can break off and float inside the joint space. This causes more pain and damage.
Unlike some other forms of arthritis, such as rheumatoid arthritis, osteoarthritis affects only joint function. It does not affect skin tissue, the lungs, the eyes, or the blood vessels.
Osteoarthritis symptoms often develop slowly and worsen over time. Signs and symptoms of osteoarthritis include:
- Pain
- Tenderness
- Stiffness
- Loss of flexibility
- Grating sensation.
- Bone spurst
Osteoarthritis is a disease of the joints. Unlike many other forms of arthritis that are systemic illnesses (conditions that affect multiple areas of the body or the entire body), such as rheumatoid arthritis and systemic lupus, osteoarthritis does not affect other organs of the body like skin tissue, the lungs, the eyes, or the blood vessels. The most common symptom of osteoarthritis is pain in the affected joint(s) after repetitive use. Joint pain of osteoarthritis is usually worse later in the day. There can be swelling, warmth, and creaking of the affected joints. Pain and stiffness of the joints can also occur after long periods of inactivity (for example, sitting in a theater). In severe osteoarthritis, complete loss of the cartilage cushion causes friction between bones, causing pain even at rest or pain with limited motion.
Symptoms of osteoarthritis vary greatly from patient to patient. Some patients can be debilitated by their symptoms. On the other hand, others may have remarkably few symptoms in spite of dramatic degeneration of the joints apparent on X-rays. Symptoms also can be intermittent. It is not unusual for patients with osteoarthritis of the finger joints of the hands and knees to have years of pain-free intervals between symptoms.
Osteoarthritis of the knees is often associated with excess upper body weight, with obesity, or a history of repeated injury and/or joint surgery. Progressive cartilage degeneration of the knee joints can lead to deformity and outward curvature of the knees, which is referred to as being “bowlegged.” People with osteoarthritis of the weight-bearing joints (such as the knees) can develop a limp. The limping can worsen as more cartilage degenerates. In some patients, the pain, limping, and joint dysfunction may not respond to medications or other conservative measures.
Osteoarthritis of the cervical spine or lumbar spine causes pain in the neck or low back. Bony spurs, called osteophytes, that form along the arthritic spine can irritate spinal nerves, causing severe pain that can radiate from the spine as well as numbness and tingling of the affected parts of the body.
Osteoarthritis causes the formation of hard, bony enlargements of the small joints of the fingers. Classic bony enlargement of the small joint at the end of the fingers is called a Heberden’s node. The bony deformity is a result of the bone spurs from the osteoarthritis in that joint. Another common bony knob (node) occurs at the middle joint of the fingers in many patients with osteoarthritis and is called a Bouchard’s node. Heberden’s and Bouchard’s nodes may not be painful, but they are often associated with limitation of motion of the joint. The characteristic appearances of these finger nodes can be helpful in diagnosing osteoarthritis. Osteoarthritis of the joint at the base of the big toe of the foot leads to the formation of a bunion. Osteoarthritis of the fingers and the toes may have a genetic basis and can be found in numerous female members of some families.
While there isn’t any single known cause of osteoarthritis, there are several risk factors that should be considered. Knowing and controlling these risk factors can help you minimize the risk or even help postpone or prevent getting OA altogether. Having risk factors for OA doesn’t mean everyone will definitely get it. No single risk factor is enough to cause OA; it is more likely that a combination of risk factors works together to cause the disease.
There are two distinct types of osteoarthritis –
- Primary
- Secondary
Primary osteoarthritis, osteoarthritis not resulting from injury or disease, is mostly a result of natural aging of the joint. With aging, the water content of the cartilage increases, and the protein makeup of cartilage degenerates. Eventually, cartilage begins to degenerate by flaking or forming tiny crevasses. In advanced osteoarthritis, there is a total loss of the cartilage cushion between the bones of the joints. Repetitive use of the worn joints over the years can irritate and inflame the cartilage, causing joint pain and swelling. Loss of the cartilage cushion causes friction between the bones, leading to pain and limitation of joint mobility. Inflammation of the cartilage can also stimulate new bone outgrowths (spurs, also referred to as osteophytes) to form around the joints. Osteoarthritis occasionally can develop in multiple members of the same family, implying a hereditary (genetic) basis for this condition.
Secondary osteoarthritis is a form of osteoarthritis that is caused by another disease or condition. Conditions that can lead to secondary osteoarthritis include obesity, repeated trauma or surgery to the joint structures, abnormal joints at birth (congenital abnormalities), gout, diabetes, and other hormone disorders.
Obesity causes osteoarthritis by increasing the mechanical stress on the joint and therefore on the cartilage. In fact, next to aging, obesity is the most significant risk factor for osteoarthritis of the knees. The early development of osteoarthritis of the knees among weight lifters is believed to be in part due to their high body weight. Repeated trauma to joint tissues (ligaments, bones, and cartilage) is believed to lead to early osteoarthritis of the knees in soccer players and army military personnel. Interestingly, studies have not found an increased risk of osteoarthritis in long-distance runners.
Crystal deposits in the cartilage can cause cartilage degeneration and osteoarthritis. Uric acid crystals cause arthritis in gout, while calcium pyrophosphate crystals cause arthritis in Pseudo-gout.
Some people are born with abnormally formed joints (congenital abnormalities) that are vulnerable to mechanical wear, causing early degeneration and loss of joint cartilage. Osteoarthritis of the hip joints is commonly related to structural abnormalities of these joints that had been present since birth.
Hormone disturbances, such as diabetes and growth hormone disorders, are also associated with early cartilage wear and secondary osteoarthritis.
Factors that increase your risk of osteoarthritis include:
- Older age – The risk of osteoarthritis increases with age.
- Sex – Women are more likely to develop osteoarthritis, though it isn’t clear why.
- Bone deformities – Some people are born with malformed joints or defective cartilage, which can increase the risk of osteoarthritis.
- Joint injuries – Injuries, such as those that occur when playing sports or from an accident, may increase the risk of osteoarthritis.
- Obesity – Carrying more body weight places more stress on your weight-bearing joints, such as your knees.
- Sedentary lifestyle – Cartilage depends on joint use for its nutrition.
- Certain occupations – If your job includes tasks that place repetitive stress on a particular joint that may predispose that joint toward eventually developing osteoarthritis.
- Other diseases – Having diabetes, underactive thyroid, gout or Paget’s disease of bone can increase your risk of developing osteoarthritis.
- Family history
Most often doctors detect OA based on the typical symptoms (described earlier) and on results of the physical exam.
X-rays are still the main diagnostic tool however arthroscopy, ultrasound, MRI, CT scan etc. are used specially for experimental studies and not recommended for routine clinical use. X-rays can show the extent of joint deterioration, including narrowing of joint space, thinning or erosion of bone, excess fluid in the joint, and bone spurs or other abnormalities.
There is no blood test for the diagnosis of osteoarthritis. Blood tests are performed to exclude diseases that can cause secondary osteoarthritis, as well as to exclude other arthritis conditions that can mimic osteoarthritis.
Ayurveda Management of Osteoarthritis
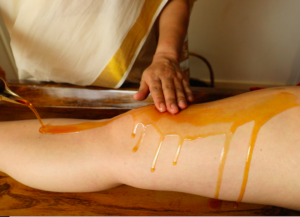
The vata (one of the three bio-regulating principles of the body) is aggravated by various reasons like improper diet, over exertion, injury, exposure to cold & intake of cold items, suppression of natural urges, staying awake at night, stress, depression etc. Apart from these, aging is a primary cause as vata predominance in body increases as age of the person advances towards old age. Individuals with the Vata Prakruti are also more prone for the Sandhivata.
Vata is rooksha (dry) in nature. When Vata get vitiated in any of the joints, dries up the lubricating synovial fluid inside the joint capsule, degenerates the joints and causes the destruction of the cartilage.
Sandhivata gradually worsens with time, and no cure exists. But Sandhivata treatments can prevent the progression of the disease, relieve pain, rejuvenates damaged cartilages, and improves the joint lubrication, function & strength.
Sandhivata treatment includes both Samana chikitsa and shodhan chikitsa. Shamana chikitsa includes Ayurveda oral medicines and external applications. Shodana chikitsa includes Ayurveda Panchakarma and Kayakalpa therapies for detoxification and rejuvenation. Healthy diet habits & life style are equally important in maintaining the joint health.
At CHARAKA, we provide very effective treatment for Sandhivata. Early diagnosis and treatment is the key to controlling Sandhivata-osteoarthritis. Panchakarma procedures require around 3 – 4 weeks depending on the joint involved and patient can expect significant benefit within this period.
Our goal of managing Sandhivata-osteoarthritis includes controlling/relieving pain, maintaining and improving range of movement and stability of affected joints and limiting functional impairment.

